
It’s a busy afternoon at the Galilee Medical Center in Nahariya. The staff of the Rehabilitation Department, which was recently converted into the Corona Department, are supervising twenty inpatients through screens and speakers. In tandem, they are facilitating the release of two patients, an operation that requires coordination with the health insurance organizations and an ambulance that will deliver them to quarantine at home.
A woman who came to the hospital with her 14-year-old son to visit her father, was informed upon her arrival that he had died. One of the nurses in the ward helps them in the fight to enter the ward and see him one last time.
Professor Masad Barhoum, director of the Galilee Medical Center, says that his hospital is over capacity and understaffed, which is taking its toll both on the mental health of his staff, and on the care of patients.
"My staff is suffering from mental scarring," he says. "They were not taught how to deal with this reality. They have trauma from saying goodbye to patients who they fail to save, from families who are not able to say goodbye to their loved ones. My workers are crying, and you don't typically see this kind of crying on the wards."
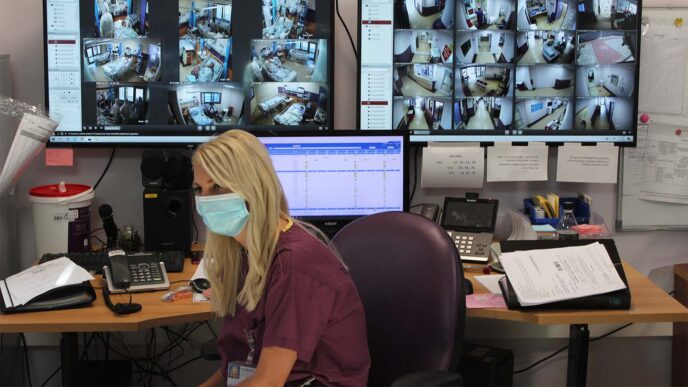
In the first wave of the virus, only two corona patients who needed respirators were treated, and only one patient died at the Nahariya hospital. About twenty patients on respirators are now hospitalized there at any given moment, and 50 patients have died since August.
"There are a lot more difficult and complex cases that can turn around in a second," says nurse Chaya Kramisi. "They go into resuscitation in the morning, we realize that there is no chance of recovery, and then we must communicate with the family."
"It's getting harder and harder, we're feeling the mental strain and starting to break under the pressure," Kramisi says. "We're used to screens now. I went in to see a patient this morning that I talk to every day. I said, 'Remember me?' – he didn’t know who I was. We can no longer embrace them, look into their eyes, be there in the way we are used to being there for the patients.”
Rika Moskowitz, the head nurse in the ward, describes the situation in simple words: "Our hearts ache all the time. I have an exemplary staff, who have a lot of heartache."

Since the beginning of the epidemic, the hospital allowed any staff member who wished to see a psychologist for mental health support. Prof. Barhoum is now initiating meetings with a psychologist for all the staff members involved in the treatment of the coronavirus. Meanwhile, the high load of corona patients continues to increase and create pressure on the staff, and Barhoum announced that he is preparing to open a fifth corona department.
“We are at war”
Staff in the other hospital units have also been affected by the coronavirus outbreak. To date, four wards have been converted to corona wards – two inpatient wards, a geriatric ward and a rehabilitation ward. For a hospital in the periphery, these are changes that have a dramatic impact on a wide circle of patients and their families.
"We are at war, and war is taking all the resources. Geriatric patients now have nowhere to go since we converted the geriatric ward to the corona ward. I received a referral from a rehabilitative patient who also needs dialysis. I tried to find them a place and failed,” Barhoum explains.
According to Prof. Barhoum, the increase in hospital activity over the past decade has not been matched by appropriate supplements to the workforce.
"We became the second largest hospital in the north, after Rambam in Haifa, but we remained small in our number of employees. We are the thinnest-staffed hospital in the government system, especially in terms of intensive care staff – ewxactly the people I need to care for the complex corona patients,” he says. “There are still neurosurgical intensive care units here, cardiology units, pediatric units, and I cannot close them because I am serving the community.”
The corona unit for respiratory patients requires one intensive care nurse, a profession which requires years-long training, per every two respiratory patients. There are currently ten intensive care nurses in the ward, which limits the number of respiratory patients the ward can treat.
"If we enter an emergency where I have to send nurses with minimal training to look after respiratory patients, I will do it. But I hope we don’t get there,” Barhoum says.
In the wake of the epidemic’s outbreak, the hospital received funding for an additional 52 nurses and 14 doctors from the Ministry of Health. According to Barhoum, however, even the supplementary medical staff will not sufficiently ease the current load.
"It's not enough, I need more," he says. "We are short 70 doctors, 100 nurses, 50 paramedical workers (radiologists, medical technologists, dietitians and more), and 114 administrative workers."

According to Barhoum, transfers of patients from overcrowded to less crowded hospitals by the Ministry of Health will not solve the congestion problems at the medical center.
"I do not have an overcrowding problem of mild and moderate corona patients," he explains. "These patients are cared for by nurses without intensive care training. In contrast, the difficult and respiratory patients, who need intensive care nurses, cannot be transferred on long trips to the center of the country."
“At first I ran away from the word ‘selection,’ but I do not want to run away from the truth”
Prof. Barhoum is concerned about the gap between the enormous burden on the hospital and the health system in general, and the mood in large sections of the public against obeying the guidelines for preventing the spread of the virus.
"People continued to hold weddings and events because they did not internalize the seriousness of the situation," he says. "There are 500 patients hospitalized in the north. It’s a lot for us, but it is not enough to overcome the Israeli mindset that says 'it will not happen to me'. Unfortunately many more people will die. Dozens a day, hundreds a month, and then maybe it will affect people. If it starts to get threatening, if anyone is at risk of infection, or if the health care system collapses and becomes a selection."
Choosing the word “selection” is not easy for him.
“I understand the connotation of the word. At first I ran away from it, but I do not want to run away from the truth. We are approaching a situation where young doctors will have to make decisions about who to save and who to leave to die,” he says. “In a multi-casualty event, the most senior doctor is sent to make the decision of who will die. When I was a young doctor, I would not be able to sleep after my patient had passed away because it creates a tremendous difficulty.”
“I constantly think about where there are overloads of patients”
Diana Kalisher, the nurse in charge of the emergency room, has been given responsibility for two more emergency rooms in recent months: a respiratory emergency room, designed for patients with respiratory symptoms suspected of having coronavirus, and an emergency room for verified corona patients.
"Overall, the activity does not slow down – there are accidents, shootings, stabbings, everything. But now, we have to additionally activate these two emergency rooms, which we have set up in our waiting rooms. As a result, there are fewer waiting rooms for emergency rooms, and more patients waiting in the corridor,” she explains. “We have to run back and forth from emergency room to emergency room. I constantly think about where there are overloads of patients."
The emergency room itself is another example of the logistical burden that the hospitalization of corona patients creates on the hospital system. Next door is a CT scan room used by the emergency patients. When a verified or suspected corona patient hospitalized in the emergency room needs a scan, they must go through the general emergency room. Any such passage requires the accompaniment of the medical staff with security personnel clearing the way. According to Kalisher, about twenty such crossings are made each day.

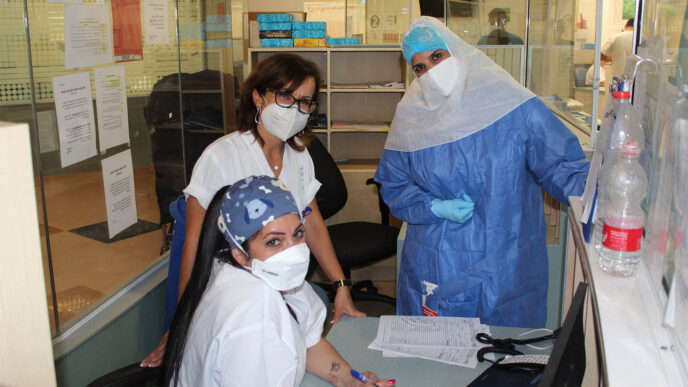
Meanwhile, in the corona ward, nurse Jacob Sobrover explains to a patient's relative, from the other side of a glass barrier, how to disinfect himself after visiting the ward.
"I have been working in the rehabilitation department for nine years and not a single patient has died," he says. "Now people are dying every day, it’s very hard."






