
"The most significant thing I have learned from the last year is humility," said Dr. Michael (Miki) Halbertal, director of Rambam Hospital in Haifa. "Coronavirus taught us humility, and those who haven’t learned have a big problem."
Halbertal, who heads the largest medical center in the north of Israel, warns that the most important lesson from the crisis has not yet been learned. Israel's public health system has been starved for years, and urgently needs an "injection of resources" to fulfill its mission, even before the corona crisis.
Davar sat down with Halbertal to hear his play-by-play account of his hospital’s developing response to the pandemic.

Halbertal (62) was born in Bnei Brak and moved with his family to Tel Aviv at the age of six. In the army, he served in the Israel Air Force's search-and-rescue unit, and when he was released, he began studying medicine at the Technion.
"Ever since I was a kid, I wanted to be a doctor. I had no other dream," he said.
He met his wife, Marin, in the army. They have four children and six grandchildren, and today they live in Zichron Yaakov. In 1986, he began working at Rambam and specialized in pediatric intensive care.
Initial reports meet reality
Halbertal recalled the first conversations about what was then called the 'Chinese virus,’ sometime in the beginning of 2020. When news began to arrive about the outbreaks of the new virus, “it seemed distant and unrelated.”
"We did not understand at all what was going to happen," he continued. "News began to arrive about what was happening in China, it seemed distant and unrelated. At some point, the Ministry of Health issued a preparation procedure, and we said to ourselves, 'Okay, there will be a few patients'. We had previous experience with the Ebola virus and SARS, which did not affect us so much in Israel. So we were pretty smug.”

A series of events over the following weeks changed his attitude towards the new virus.
"The insights deepened with the story of the Israelis on the ship in Japan, when it was clear that there would be corona patients entering Israel. At the same time, we began to hear more and more what was happening around the world, especially in Asia,” he said. “Little by little the stories started coming from Western Europe. Then we heard what happened in Italy, and we understood that we needed to prepare.”
What were the first steps you took?
"The ramp up was gradual. The first step was to allocate ten high-pressure isolation rooms that we have in the hospital for the treatment of corona patients. We quickly realized that this would not be enough. We would need larger areas."

"Then came instructions from the Ministry of Health, and we began to prepare according to what they told us. They asked us to prepare a hospital ward with 30 beds, including four intensive care units. The hospital management met and chose a building that could be insulated in terms of air conditioning and entrances. It quickly became clear that it was not enough, and we moved on to establish two more departments."
Understanding the magnitude of it all
Another milestone that Halbertal pointed out was when the Ministry of Health published a document that warned of thousands of cases of severe coronary heart disease in Israel and considerable mortality.
“When we saw that, it gave us a ballpark estimation for the intensity we are preparing for, and that brought us down to earth,” Halbertal said.
"We understood that this was a very significant event, and that we needed to come together and find solutions. It was definitely very worrying. Did we then think it would be an event of over a year and so powerful? No. But we realized it would not be an easy and fleeting event."
At that point, preparations became more intense.
"We realized it was going to take up a lot of our time as the hospital management. We started delegating things, we built work processes, work procedures. We were getting most of our information from Europe," he continued.
One of the major concerns, beyond how patients were to be treated, was around hospital staff members and how to protect them from infection.
"From the data we received, many hospital personnel in the world were infected. The question arose as to how we protect our staff. The situation had a lot of layers. Despite the size of Rambam, and even though there are 5,700 employees here, I personally know most of the people who work here. It's a family,” he said.
"So we did a lot of preparatory work in building the protocols, and we tried to understand how to protect the employees."
Leading the staff: "I realized that the whole hospital needs to be prepared”
Beyond organizing and writing the procedures, Halbertal's major task was to harness the efforts of thousands of hospital staff to deal with the new needs and changing realities.
"It was a complex event every step along the way," he said. "When we started opening the internal medicine wards, we turned to staff and asked for volunteers. There was no understanding of what the extent of this incident would be, we thought it was a short term event. Very quickly, we realized it was not enough. We needed everyone to be committed to this purpose."
How did you understand that?
"There was an incident where we needed a few staff members on an as-needed basis to care for coronavirus patients. We turned to some intensive care staff and they said, 'wait, we did not volunteer. Why us?'"
What did you do?
"I turned to the staff and said that we are all afraid, that I am also afraid, that there are a lot of unknowns. And on the other hand, we are here to provide medical services, and to give answers as is expected of us. I said all the people who feel for some reason that they cannot deal with it, let them say so, so we know where we stand.
"I'm not talking about someone who can't for objective reasons like a medical condition, but about concerns. I said that I, as the one who runs the team, I need to understand who is with me and who is not. And as I expected, no one asked to be exempt."
How do you keep staff members from burning out in the face of this intense reality and uncertainty?
"Almost since the beginning, we have provided mental and emotional support services for staff members. In addition, I would pass on information constantly. Once a day, twice a day, I would update what the decisions were, what the issues were, what the data was. When people understood what was going on inside the hospital, it was much easier for them to connect.
"In addition, the entire hospital management and I were very connected to the staff. We walked around all parts of the hospital, and we met the staff all the time."
Halbertal emphasizes that as the pandemic lengthened, it was the involvement of all hospital staff that made it possible to survive.
"We have realized that we were actually in a disaster that lasted a year," he said. "Maintaining this level of preparedness for an entire year is not an easy task. War is a month. In the event of a casualty, the surgical side of the hospital takes control. Here, because it is a disease, the internal wing had to take it on.

"But we realized it was not just on the internal wing. So ophthalmologists, orthopedists and nurses from all departments came to help. There was no other way. If we didn’t get the entire hospital involved, it would have been impossible to deal with such an event," Halbertal explained.
For Halbertal, the commitment of his staff is one of the best things that came out of the past year.
"These are 5,700 people who come and ask how we can do better," he said proudly. "I'm not just talking about the personnel who chose to be therapists, where this attitude is expected. The maintenance, communication and other teams mobilized and did whatever was needed."
"I always say that over the course of my life, I have found two exciting organizations – Rambam and Kibbutz Kishor," Halbertal said excitedly. He refers to the kibbutz near Karmiel, which is intended for people with disabilities. He has an intimate acquaintance with the place.
In the 1980s, while his family was living in Canada, his daughter was involved in a car accident and was rushed to the hospital where he specialized in pediatric intensive care. He cared for her and saved her life but "there was a severe head injury, and to this day she lives with a disability."
When she grew up, she joined Kibbutz Kishor, which also includes her parents, who even have a home there so they can be close to their daughter.
"There are 180 people there with special needs, and that is their home," he explained
Establishing an underground facility: "Within three days we were operating"
At the beginning of September, Rambam's management made the dramatic decision to turn its emergency underground compound into a coronavirus ward. The corona wards that already operated at the hospital were moved underground, and additional wards manned by soldiers from the medical corps were set up. Halbertal describes how the decision was made.
“During the second wave, our internal medicine wards could accommodate for 80-90 patients, and at the time we had already reached that number,” Halbertal said. "All over the country, there were 15,000 confirmed cases a day, with a positive testing rate of 15% or more, especially in the north, in the Arab population. We realized that, as the center of the northern region of Israel, we could not withstand it.
"We debated for a long time, because there would be a lot of ripple effects for the staff, and also logistical challenges. We did not receive instructions from the Ministry of Health. We decided on it out of commitment to our patients, we said there can be no situation where we do not give them solutions."

"We made the decision right after Rosh Hashanah. It was Monday morning. When I asked how long it would take to get organized. I was told ten days to two weeks. I said 'fine'. By Thursday at 2 pm, after three days, everything was ready for the first ward to operate. It goes back to the staff, to their commitment to do the unbelievable in a short period of time," Halbertal said.
The cooperation with the army was unique, and not to be taken for granted.
"It was clear that in order to operate the underground hospital we needed more human resources,” he explained. “We tried to think of all sorts of solutions, like combining hospitals and assembling the required manpower that way, and then we started talking about the military. But for a number of reasons we couldn't pull it off.
"When we entered the second wave, I was able to convince the chief medical officer to work together with us. It’s very unusual in Israel for army and civilian systems to cooperate. But we got a very skilled team."
In the field: "When you looked at the patients, you saw the loneliness"
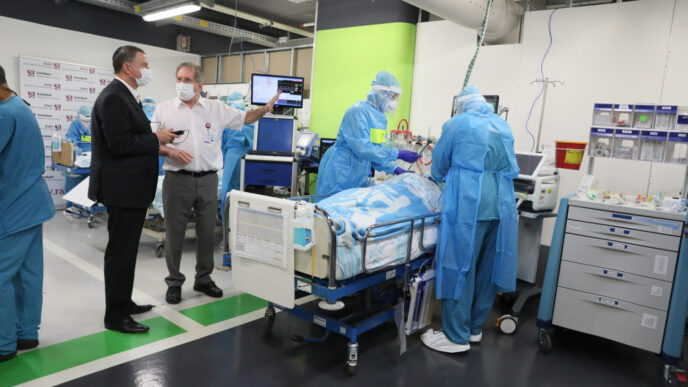
The construction of the facility, and the cooperation with the medical corps, put Rambam in the headlines. The prime minister, the defense minister and the health minister came to visit.
"When you enter this underground structure, it is exciting in its power, in the magnitude of the solutions it created. But when you walked around there and looked at the patients, you saw the loneliness. The people left there alone. About 2,000 people passed through this facility and 300 died. It's terrible,” Halbertal said.
A moment of simple humanity encountered in the facility stays with him.
"When we brought in the army and brought the paramedics, there was a 92-year-old man in one of the beds, who was at the end of his journey. One of the paramedics sat down next to him and just held his hand."
Two weeks ago, Rambam's management decided to close the facility, after almost half a year of continuous operation.
"There was a lot of deliberation about whether to close. These are decisions in an age of uncertainty," Halbertal said. "We waited to see what would happen on Purim, because we were very afraid of it. We waited to see what effect the vaccine would have. In the second wave, as soon as we entered the lockdown, the effect was very significant and we saw the decrease in morbidity here in the north.
"In the third wave, the lockdown effect was very weak. We had a large number of patients and the quarantine did not have much effect. Then a drop started, mainly because of the rising amount of vaccines. We waited two weeks after Purim and then made the decision. In the end, being in an underground hospital for five months is not great fun."
Lessons learned: "We need to change the paradigm and invest in social services"
Along with admiring the effort and sacrifice of Rambam workers during the pandemic, Halbertal has vital insights into the price of neglecting the health care system, and the general necessity of greater investment in health services.
"We came into the pandemic very unprepared. Just so you understand, in February 2020 when we started there was a nationwide supply of 110 ventilators, 80 of which did not work because they were not serviced,” he explained.“The Ministry of Health's emergency department functioned without a manager for many years."
What is the root of the problem in your opinion?
"The gap between authority and responsibility. The authority to allocate the resources is in a place with zero responsibility for the health situation in the country, in the Ministry of Finance. However, all the responsibility is with us, with very little authority. This is very problematic.
"The numbers speak for themselves. Expenditure on health up to the last year is a stable 7.4 percent of GDP. We see the effect of this in the overcrowding of hospitals and in the low rates of doctors and nurses in Israel relative to the population. We are constantly on the verge of collapse – on a daily basis, regardless of such a large event like the pandemic."
Do you see a change on the horizon?
"No. And that's what's so unfortunate. We've been through this year, and you start to think ahead and see that no one has learned their lessons. We worked really hard, so we succeeded despite the situation Israel's health system was in. We survived it, so now the idea is ‘let's just go on like this.’ We need to instead learn that the health system needs to look different, we need a different vision. If we don’t do that, it will be a very significant mistake that our children will pay the price for."
For Halbertal, investing in health care is part of a broader concept.
"It's not that the only thing that has problems in the State of Israel, the health care system. But you have to understand that when you look at the state, the existential danger comes from the deterioration of services to the citizen, of which health is a part. The same is true of welfare, police, and the courts.
"It's not that I'm ignoring the security issue. But I think we need to change the paradigm, and understand that we need to invest in social services. It should be safer to walk the streets, drive on the roads, express our opinions, and get health services."
What are the most urgent actions to take, in your opinion?
"The system needs an injection of resources. We cannot bridge the gaps without it. It has to happen logically, in an orderly fashion. It is impossible to continue the way we were, to keep the system hungry, and medical professionals like gladiators in some amphitheater, with the authorities watching us fight amongst ourselves for the meager resources.
"Israel is not a big country, but it is aging fast, and that has impact in terms of medicine. If Israel as a democratic society decides that health is a right of its residents, there is no choice but to invest in the healthcare system.”
What goal would you set?
"There can be no hospitalizations in the hallway. We do wonderful things, but as long as there are patients treated in the hallway [due to lack of beds and rooms], then we have done nothing. It has nothing to do with medicine, it has to do with human dignity. No one would want to get medical treatment in the hallway."
Halbertal also thinks Israel needs to establish a supervisory body for all hospitals in the country.
"The delay in establishing such an authority is a mistake we are paying for every day. Until now, for example, we have not been able to regulate patient loads. The first wave, for example, was crowded in Jerusalem and the center, while we had almost no patients. I offered to take more, but it didn't work. Then suddenly I had too many and it was the same story.
"We need to live with coronavirus for quite some time, and things can change. We need to be prepared for an outbreak to start somewhere and there needs to be regulation throughout the system."
According to Harbetel, home hospitalization also needs to be improved.
"We understood that traditional medicine will have to change. The thought has been that in order to treat a patient, you have to touch him and smell him. All that is important in some cases, but even virtual medicine can solve a lot of issues and it could significantly improve the Israeli health system,” he said.
“In between general practitioners and hospitals, we also need to upgrade and empower the inpatient capabilities of community medicine facilities. That is not to replace the hospitals. The hospital needs to take care of the more complex patients who need to be there.”
Personal memory: "Miki, take care of me"
When asked about a person or an event that affected him over the past year, Halbertal recalls two stories.
"Recently we had a number of mothers in critical condition, all on ventilators. These are very, very complex cases. A 35-year-old woman came to us with an 'expensive' pregnancy – her first pregnancy after In-vitro fertilization at week 25 and in a difficult situation. Saving her and rescuing her fetus was a crazy operation, and we succeeded. Seeing her go visit her baby after she recovered, and walk in here, to the executive offices, it was extremely exciting. That is an extreme story, but there were a lot like that.
"A second story that stays with me me is a conversation with our chief respirator technician. As an intensive care physician, I’ve worked with him from my first day here. And he contracted coronavirus. I heard he was home, barely able to speak, and they brought him here. I came to visit him and he said 'Miki, Save me. Take care of me.' It was really significant for me, to understand this disease on the one hand, and the impact it had on the family, the Rambam family. He recovered in the end. But those who died will not be able to return."






